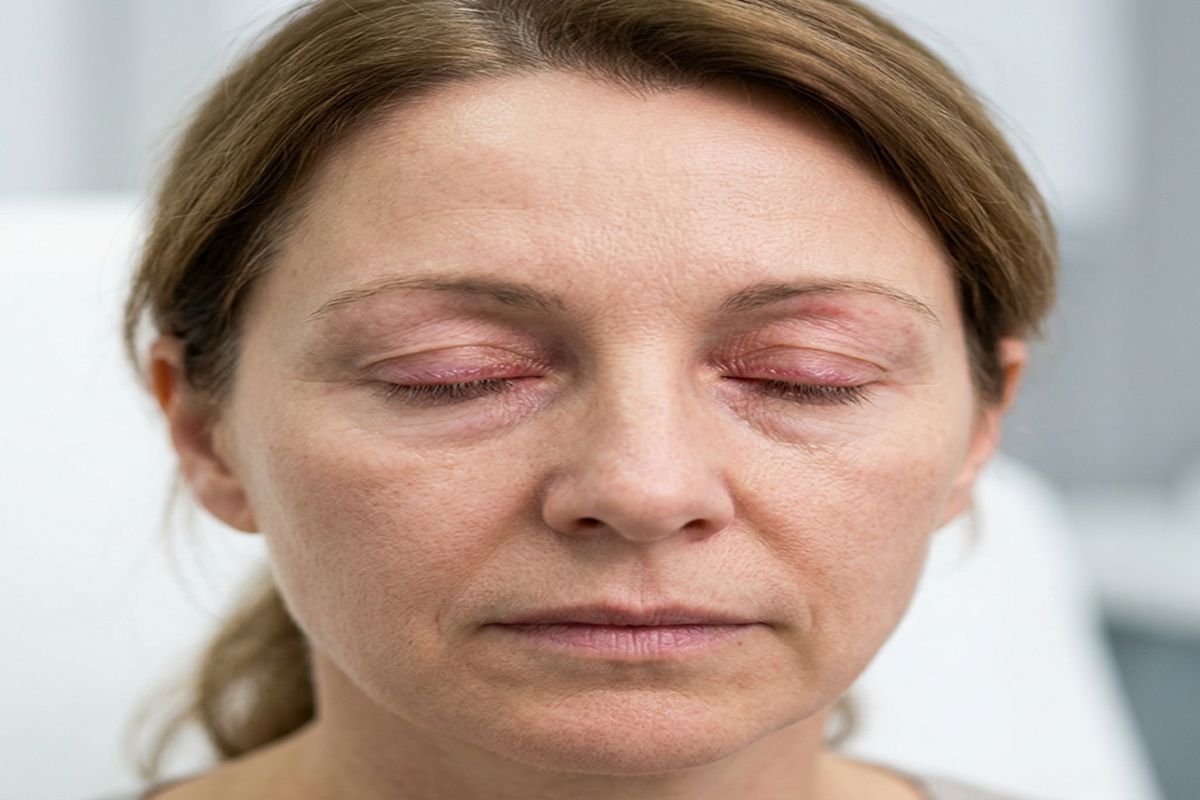
Ocular rosacea is inflammation of the eyelid margins and the surface of the eye, a subtype of rosacea that many people don’t know exists until they’re diagnosed. It causes dryness, burning, foreign body sensation, intermittent redness, and light sensitivity. It also makes the eye area reactive to triggers that most people never think about, including everyday eye makeup.
The good news: ocular rosacea doesn’t mean giving up eye makeup. It means being thoughtful about what goes near your eyes.
What Is Ocular Rosacea?
Rosacea is a chronic inflammatory skin condition. When it affects the eye and eyelid area, which occurs in an estimated 60% of people with cutaneous rosacea, and sometimes without any visible skin rosacea, it’s classified as ocular rosacea.
Key features:
- Meibomian gland dysfunction (MGD): The oil glands in the eyelid margins can become blocked, reducing the lipid layer of the tear film and causing dry eye symptoms
- Blepharitis: Inflammation along the eyelid margin, often with crusting or scaling at the lash base
- Conjunctival redness: Persistent pinkness of the eye white (sclera)
- Sensitivity to products and environments: Fragrances, smoke, wind, and certain skincare actives commonly trigger flares
Ocular rosacea is managed, not cured. Identifying and avoiding personal triggers is the foundation of management.
Makeup Ingredients That Commonly Trigger Ocular Rosacea Flares
Fragrance
Fragrance is the most common irritant in cosmetics for people with sensitive eyes. Eye products are particularly problematic because even trace amounts near the tear film can cause burning. Choose: look for “fragrance-free” specifically, “unscented” products may still contain masking fragrances.
Preservatives (especially BAK)
Benzalkonium chloride (BAK) is a preservative found in some eye drops and occasional cosmetic formulations. It disrupts the tear film’s lipid layer and is known to worsen meibomian gland dysfunction, the specific mechanism that causes many ocular rosacea symptoms. Check: ingredient lists on mascara and eyelid primers specifically.
Alcohol and Acetone-Based Makeup Removers
These dissolve eye makeup effectively but strip the lipid layer from eyelid skin. For people with ocular rosacea who already have a compromised meibomian gland function, further disruption of eyelid surface oils worsens tear film instability. Swap: micellar water or a gentle oil cleanser (like squalane or fractional coconut oil) for eye makeup removal.
Kohl and Kajal Liners
Traditional kohl and kajal formulas are applied inside the waterline, depositing product directly on the lacrimal margin. Research has shown these formulas migrate into the anterior eye more significantly than other liner types, and their carbon black or antimony sulfide base can accumulate in the meibomian glands, worsening blockages.
Avoid: all waterline liner when managing ocular rosacea.
Waterproof Era Mascara (Standard Polymer Formulas)
The solvents required to remove waterproof mascara, typically acetone or oil-based removers, require rubbing near the lash margin. This mechanical irritation can worsen blepharitis and disturb the oil glands along the lash base.
Safer Makeup Choices for Ocular Rosacea
Tube Mascara
Tube mascara is consistently the recommended choice for people with ocular rosacea and blepharitis. The polymer tubes encasing each lash don’t shed particles, don’t smear, and rinse off cleanly with warm water, eliminating the need for heavy removers and the rubbing motion that aggravates lid margins.
Fragrance-Free, Ophthalmologist-Tested Products
Several mascara brands produce ophthalmologist-tested, fragrance-free formulas specifically marketed for sensitive eyes. These are the natural starting point. Reading the formulation list for fragrance derivatives (linalool, citronellol, benzyl alcohol, these are fragrance compounds often listed separately from the word “fragrance”) is worth the extra time.
Powder Eyeshadow with Minimal Fallout
Pressed powder eyeshadows with dense, low-fallout formulas are generally well-tolerated when applied with a brush and kept above the crease line, away from the lash margin and waterline. Avoiding shimmer and glitter particles near the lower lash line reduces particle migration into the tear film.
Cream Eyeshadow for the Lid
Cream eyeshadows applied to the lid (not near the lash line) have limited contact with the tear film. They also eliminate the particle fallout associated with powder application over the eye.
Application Technique Adjustments
Avoid the waterline entirely. The most common trigger for flare-ups specifically tied to makeup is product on the waterline. Skip it completely. There are no safe waterline liner options for active ocular rosacea, even “ophthalmologist-tested” products at the waterline are riskier than the same products on the outer lash line.
Keep liner on the outer lash line only. Gel liner applied precisely to the outer upper lash line has much less tear film contact than any waterline application, and is generally well-tolerated with ocular rosacea.
Apply mascara away from the lash root. Starting mascara application 1-2mm from the base of the lash (rather than against the root) reduces product contact with the oil glands along the lash margin.
Use a clean brush for every application. Blepharitis associated with ocular rosacea involves bacterial colonization of the lash margin (most commonly Staphylococcus epidermidis and Demodex mites). Reusing brushes without cleaning between uses reintroduces these bacteria to the eye area. Clean brushes after every use for eye tools used near the lash line.
Makeup Removal for Ocular Rosacea
Remove makeup gently, without rubbing. Press a soaked cotton pad against the closed eye and hold for 10-15 seconds before swiping. The soaking period dissolves product; rubbing motion should be minimal.
Micellar water: effective and gentle for sensitive eyes. Choose a formula without alcohol or fragrance.
Squalane or diluted fractional coconut oil: for any products that don’t come off with micellar water. Apply with a cotton pad, let sit briefly, then wipe. These don’t disrupt the lipid barrier the way acetone-based removers do.
Don’t skip lid hygiene. Many ophthalmologists recommend daily eyelid hygiene for ocular rosacea patients, lid scrubs or diluted baby shampoo applied along the lash base with a cotton round, as part of meibomian gland maintenance. This routine is separate from makeup removal but important to maintain even on days you wear makeup.
When to See a Doctor
If you experience any of the following, see an eye care provider before continuing makeup use:
- Vision changes alongside redness or irritation
- Corneal clouding or persistent sensitivity to light
- Eye pain (as distinct from surface irritation)
- Symptoms that don’t respond to trigger elimination
Ocular rosacea can, without management, progress to corneal involvement (rosacea keratitis), which can affect vision. If yours is more than mild, a diagnosis and treatment plan from an ophthalmologist or dermatologist, potentially including antibiotics (oral doxycycline or topical azithromycin), makes managing triggers, including makeup, much more straightforward.
Sources
- American Academy of Ophthalmology, Ocular Rosacea patient guidelines (2024)
- Geerling, G. et al. “The International Workshop on Meibomian Gland Dysfunction.” Investigative Ophthalmology & Visual Science, 2011
- Two Adv. et al. “Cosmetic contamination and ocular surface in blepharitis.” Contact Lens & Anterior Eye, 2019
- Yazici, A., et al. “Cosmetics and the lid margin.” Arquivos Brasileiros de Oftalmologia, 2020
- Rosacea Society, Ocular rosacea subtype clinical description and management summary (2023)
Our Rigorous Testing & Review Methodology
At eyeshadowlooks.com, we take our responsibility to our readers seriously. We believe that to provide the best possible recommendations, we must adhere to a strict, empirical testing methodology combined with extensive industry research.
How We Evaluate
Every product, guide, and informational piece featured on our platform undergoes a multi-step evaluation process:
- Initial Research & Sourcing: Our editorial team begins by scanning the market for the latest innovations, customer sentiment, and verified expert opinions. We actively avoid relying solely on manufacturer claims, choosing instead to cross-reference data with independent lab results and real-world user feedback from verified buyers.
- Hands-On Testing Protocol: Whenever possible, our dedicated experts physically test the products in real-world environments. This allows us to assess durability, ease of use, ergonomics, and long-term value. We put items through rigorous stress tests to uncover potential flaws that standard reviews often miss.
- Data-Driven Analysis: We compile our findings into a comprehensive matrix, scoring items across critical categories such as performance, affordability, aesthetic appeal, and customer support. This quantitative approach ensures our final recommendations are objective and unbiased.
- Continuous Monitoring: The market is always changing. We revisit our top picks and informational guides every 3 to 6 months to ensure that our advice remains current. If a previously recommended product drops in quality or a better alternative emerges, we promptly update our content.
Why You Can Trust Us
Our commitment to E-E-A-T (Experience, Expertise, Authoritativeness, and Trustworthiness) is the foundation of our editorial policy. We do not accept paid placements for our top recommendations. Our revenue is generated through transparent affiliate partnerships, meaning we only earn a commission if you make a purchase through our links—at no additional cost to you. This structure aligns our success directly with your satisfaction.
Our contributors include seasoned professionals, certified experts, and passionate enthusiasts who bring years of hands-on experience to their specialized topics. We mandate that all claims are backed by authoritative sources, which we link to whenever applicable.
If you ever have questions about our methodology or spot an inaccuracy, we encourage you to reach out via our Contact page. We are dedicated to continuous improvement and always welcome community feedback to refine our editorial standards.
Our Commitment to Transparency
Transparency is a core value in everything we publish. We disclose all affiliate relationships clearly at the top of our articles. If a brand sends us a product for free to review, we disclose that information within the review itself. However, accepting a free product never guarantees a positive review. Our allegiance is strictly to our readers. We regularly publish cautionary reviews for products that fail to meet our high standards, regardless of the brand’s industry standing or potential commission rates.
Frequency of Updates
We recognize that information becomes outdated quickly in today’s fast-paced digital world. Therefore, our team conducts quarterly audits of our most popular guides and reviews. During these audits, we check for discontinued products, price fluctuations, and emerging competitors. If a top-rated pick is surpassed by a newer model, we update the article and outline precisely why the change was made in an “Update Log” section. This dedication to freshness ensures that whenever you land on one of our pages, you are reading the most accurate and up-to-date information available.
Related Reading
Get weekly eye care & beauty tips
Expert-researched guides delivered to your inbox. No spam, ever.
Frequently Asked Questions
Can you wear eye makeup if you have ocular rosacea?
Yes, but with careful product selection. Many people with ocular rosacea wear eye makeup without triggering flares. The key is avoiding products with known irritants (fragrance, preservatives like BAK, alcohol-based formulas), using minimal products near the waterline, and practicing strict hygiene to prevent meibomian gland blockage.
What mascara is best for ocular rosacea?
Tube mascaras designed for sensitive eyes are the best choice for ocular rosacea. They don't flake, shed fibers, or smear into the tear film. Avoid waterproof mascaras that require heavy-duty makeup removers, the removal process itself can aggravate already-inflamed lid margins.
Does eye makeup make rosacea worse?
Certain products can trigger or worsen flares: fragrance-containing eye products, waterproof formulas requiring oil-based removers applied near the lash margin, kohl or kajal applied to the waterline, and makeup with glitter that sheds particles into tears. Switching to fragrance-free, minimal-ingredient products usually allows continued makeup use without worsening symptoms.